There is a dangerous relationship between diabetes and fungal infection that most patients never hear about in their doctor’s office.
When blood sugar rises too high, it does not just harm your heart, kidneys, or eyes.
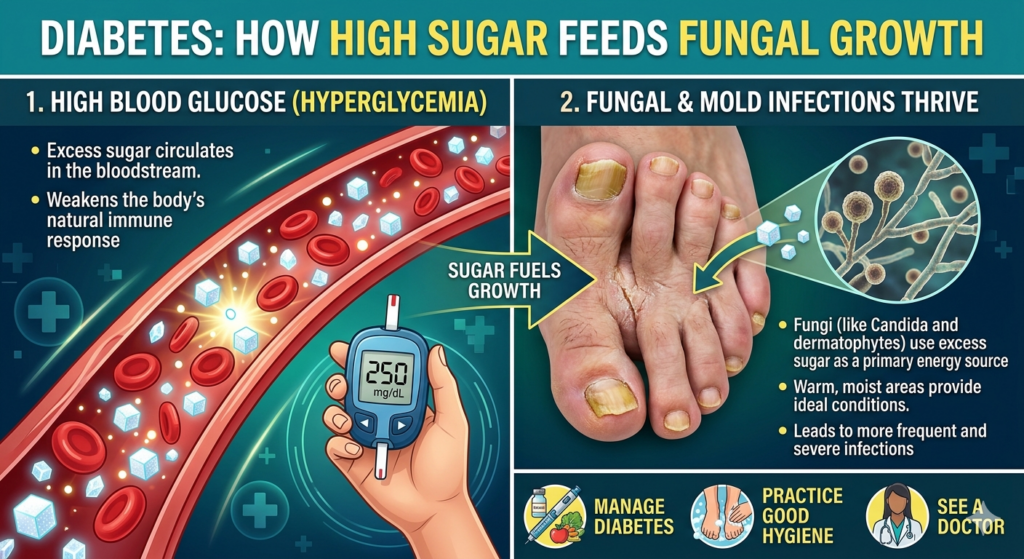
It literally feeds the molds and fungi living in and around the human body — turning the bloodstream into an all-you-can-eat buffet for dangerous organisms.
For people living with diabetes, this connection is not just interesting biology. It can be a matter of life and death.
Fungal infections that would barely register as a concern in a healthy person can become fast-moving, tissue-destroying emergencies in someone with poorly controlled blood sugar.
And when that same person lives or works in a water-damaged building, the risks multiply in ways that medicine is only beginning to fully understand.
This article investigates the science behind why sugar feeds fungi, what happens to the immune system when glucose levels spike, and why mold-exposed diabetics face a uniquely dangerous double threat.
A 2024 review in The Injector medical journal summarized the clinical reality clearly: “Diabetic patients are particularly susceptible to fungal infections because their vascular and immunological systems are compromised.”
The combination of poor circulation, nerve damage, weakened white blood cells, and glucose-rich tissue creates conditions no antifungal drug can fully offset if blood sugar remains uncontrolled.
The American Diabetes Association (ADA) has also noted that fungal infection in diabetics is a recognized clinical pattern:
“The culprit in fungal infections of people with diabetes is often Candida albicans. The only treatment is to bring blood glucose levels under control.”
Research from Penn State University published in mBio (2024) found that “metabolic diseases, like Type 2 diabetes, are associated with compositional shifts in the human gut microbiome, including the fungal fraction called the mycobiome.”
The research team analyzed over 1,000 gut microbiome samples and found that “increased Saccharomyces was linked to increased fasting blood glucose, high levels of which are a proxy for diabetes.”
A separate 2023 study published in Nature Communications concluded that “gut mycobiota play an important role in the progress of T2D.”
This creates a troubling loop: diabetes worsens the gut fungal environment, and a disrupted gut fungal environment may worsen metabolic disease.
The Diabetes and the Environment resource maintained by researchers notes that “long-term exposure to ochratoxin A, a widespread toxin found on food or in water-damaged houses, causes higher blood glucose levels, lower insulin levels, and pancreatic damage in rats.”
Ochratoxin A is produced by Aspergillus and Penicillium species — molds commonly found in water-damaged buildings.
According to Natural Awakenings (2024), “mycotoxins cause stress in the body which can create higher cortisol levels which can lead to an increase in glucose and A1C and could result in insulin resistance and pre-diabetes.”
The clinical practitioner at Sinusitis Wellness explains the mechanism further:
“Increased toxicity leads to increased cell membrane resistance, which then leads to increased insulin production but poor utilization of that excess insulin, which leads to higher blood sugar levels, and so the cycle goes.”
A preliminary study from Poland found that “mold and bacteria levels in the air were associated with an increased incidence of type 1 diabetes.”
Researchers also documented a case in which a family’s exposure to toxic mold in a water-damaged home was potentially linked to a 7-year-old child developing type 1 diabetes shortly after a major mold remediation that disturbed toxins throughout the house.
Research published in PMC (2020) adds another dimension: “Exposure to the metabolite products of indoor air molds can cause the development of autoimmune thyroidal disease and type I diabetes mellitus.”
This suggests that mycotoxins from common indoor mold species may, in some individuals, trigger the autoimmune cascade that destroys insulin-producing beta cells in the pancreas.
According to a 2009 study, “C. albicans is able to detect and respond to the levels of glucose present in the blood during disseminated hematological infections.
Dietary glucose enhances C. albicans colonization and invasion.” In other words, sugar does not just passively support fungal growth — it actively triggers the organism to colonize and invade.
The same study found that when glucose is available, C. albicans actually boosts its own stress resistance, making it harder for immune cells to kill.
Research from Southern China published in PMC examined invasive fungal disease specifically in Type 2 diabetes patients and found that “Candida albicans, Cryptococcus neoformans, and Aspergillus fumigatus were the leading agents.”
The study confirmed that “the risk of mycoses increases 1.38-fold in patients with diabetes.” Prolonged hyperglycemia was associated with unfavorable outcomes.
A 2025 review published in Microbiology Journal put it plainly: “Elevated blood glucose levels can impair the immune system and create an environment that promotes fungal growth. High glucose levels can lead to increased glycation.”
Glycation — the process where glucose attaches to proteins and lipids — disrupts the immune system’s ability to mount an effective defense, leaving the body vulnerable to fungal pathogens that would otherwise be held in check.
Diabetes mellitus creates two serious problems: elevated blood sugar (which promotes fungal growth) and poor immune cell function.
Mucormycosis — one of the fastest and most lethal fungal infections known — disproportionately strikes diabetic patients.
Research published in 2025 found that invasive fungal infections were significantly more prevalent in patients with overt hyperglycemia at 26.1%, compared to 13.9% with mild hyperglycemia and only 6.4% in normal glucose patients.
Sepsis-related mortality was highest in those with overt hyperglycemia.
Mucormycosis in uncontrolled diabetic patients carries mortality rates approaching 50–100% in disseminated cases.
In pediatric populations with disseminated mucormycosis, the overall mortality rate was 100%.
Sugar on the Skin: The Superficial Threat
High blood sugar does not only affect what happens inside the bloodstream.
It changes the chemistry of the skin itself — one of the body’s first lines of defense against mold and fungi.
A 2026 review published in PubMed covering 178 studies found that “up to 70% of diabetic patients have skin lesions due to deterioration in the skin barrier and changes in the physiological pH of the skin, leading to alterations in both innate and adaptive immunity, which predisposes individuals to bacterial, fungal, and viral infections.”
The pH shift in diabetic skin creates a less acidic environment — one where fungi like dermatophytes (the organisms behind athlete’s foot and ringworm) and Candida thrive.
The three most commonly documented superficial fungal infections in diabetic patients are tinea (dermatophyte infections), candidiasis (yeast infections), and non-dermatophyte mold infections (NDMs).
These infections frequently begin at the feet and nails, then spread — especially in patients with neuropathy who may not feel the early warning signs of infection.
Prevention and Practical Steps for Diabetics in Mold-Prone Environments
If you or someone you care for has diabetes — or pre-diabetes — and lives or works in a building with a history of water damage or mold, the following steps are essential.
Control blood glucose aggressively.
The single most important protective step is keeping A1C below 7%. Proper glycemic control reduces fungal growth conditions, improves immune cell function, and lowers iron availability that feeds dangerous molds like Mucor and Rhizopus.
Inspect your home for water damage.
Any area that has experienced a leak, flood, or chronic moisture is a potential mold site. Look for discoloration, musty odors, or visible growth on walls, ceilings, and under sinks.
Test the air quality.
Air sampling by a certified indoor environmental professional (IEP) can identify whether elevated fungal spore counts are present, even when mold is not visibly obvious.
Act on any fungal skin infections immediately.
Diabetics should not wait on athlete’s foot, nail fungus, or skin rashes. These superficial infections can become serious if blood supply and immune response are already compromised.
Watch for respiratory symptoms after potential exposure.
Coughing, facial pain, sinus pressure, or fever in a diabetic who has been exposed to water damage or mold warrants prompt medical evaluation.
Avoid disturbing suspected mold without protection.
Remediation of water-damaged material can release large numbers of spores and mycotoxins. Use N95 masks or higher protection, and consider hiring certified mold remediation professionals.
Request mold testing if you develop unexplained metabolic changes.
If blood sugar is becoming increasingly difficult to control without an obvious cause, mycotoxin exposure should be considered as a contributing factor.
Conclusion
Most people think of mold as an external threat — something living on walls or in air ducts. But fungi also live inside the human digestive system as a permanent part of the gut microbiome.
In diabetics, that internal fungal ecosystem is thrown dangerously out of balance.
The relationship between diabetes and fungal infection is one of the most underappreciated dangers in environmental health.
Sugar feeds fungi — not as a metaphor, but as a demonstrable biochemical reality documented in dozens of peer-reviewed studies.
When blood glucose rises in a diabetic patient, it creates the perfect growth medium for Candida, Aspergillus, Mucor, and other opportunistic organisms, while simultaneously dismantling the very immune cells the body needs to fight back.
For those living in water-damaged environments, the risk compounds dramatically.
Mycotoxins from indoor mold species can further damage insulin regulation, worsen inflammation, and potentially accelerate the progression of metabolic disease.
This creates a vicious, self-reinforcing cycle that neither a doctor nor a mold inspector working alone can fully address.
Protecting yourself requires both sides of the equation: controlling blood sugar with the discipline it deserves, and taking the environment seriously as a biological threat.
When one is neglected, the other pays the price.
References
-
Elizondo-Elizondo, M. et al. “Superficial fungal infections in patients with diabetes.” PubMed, 2026. https://pubmed.ncbi.nlm.nih.gov/41472504/
-
Khanna, M. et al. “Risk of Mucormycosis in Diabetes Mellitus: A Systematic Review.” Cureus, 2021. https://pmc.ncbi.nlm.nih.gov/articles/PMC8592794/
-
Al Balushi, A. et al. “Mucormycosis: An Opportunistic Fungal Infection.” PubMed, 2022. https://pubmed.ncbi.nlm.nih.gov/35533833/
-
Artis, W.M. et al. “A mechanism of susceptibility to mucormycosis in diabetic ketoacidosis: transferrin and iron availability.” Diabetes, 1982. https://pubmed.ncbi.nlm.nih.gov/6816646/
-
Brown A.J.P. et al. “Glucose Promotes Stress Resistance in the Fungal Pathogen Candida albicans.” PMC, 2009. https://pmc.ncbi.nlm.nih.gov/articles/PMC2777113/
-
Van Syoc, E. et al. “Type 2 diabetes treatment found to impact fungal community in human gut.” Penn State / mBio, 2024. https://www.psu.edu/news/research/story/type-2-diabetes-treatment-found-to-impact-fungal-community-human-gut
-
“Opportunistic invasive fungal disease in patients with Type 2 diabetes.” PMC, 2019. https://pmc.ncbi.nlm.nih.gov/articles/PMC7232281/
-
“The Roles of Autoimmunity and Biotoxicosis in Sick Building Syndrome.” PMC, 2020. https://pmc.ncbi.nlm.nih.gov/articles/PMC7345570/
-
“Microbial toxins and Diabetes.” Diabetes and the Environment. https://www.diabetesandenvironment.org/home/environmental-chemicals/microbial-toxins
-
“The Link Between Mold Exposure, Blood Sugar and Weight Gain.” Natural Awakenings, 2024. https://www.naturalawakeningsboston.com/2024/12/31/517375/the-link-between-mold-exposure-blood-sugar-and-weight-gain
-
“Weight Gain, Insulin, and Leptin Resistance Post Mold Exposure.” Sinusitis Wellness, 2022. https://www.sinusitiswellness.com/weight-gain-insulin-and-leptin-resistance-post-mold-exposure/
-
American Diabetes Association. “Diabetes and Skin Complications.” https://diabetes.org/about-diabetes/complications/skin-complications
-
“Impact of Diabetes Mellitus on Fungal Infections.” Microbiology Journal, 2025. https://microbiologyjournal.org/the-impact-of-diabetes-mellitus-on-fungal-infections



0 Comments