When people think about blood clots, they usually blame surgery or sitting too long. But studies are showing mold, yeast, and fungal infections may be part of the story too.
Whether it is Aspergillus invading the walls of blood vessels, Candida hijacking the coagulation cascade, or mycotoxins from water-damaged buildings disrupting platelet behavior, the connection between fungal biology and blood clotting is real, documented, and underappreciated by both patients and many clinicians.
This article explores the mechanisms behind fungal-related thrombosis, what the research says, and why anyone dealing with mold exposure should understand this risk.
Scientists and clinicians have long observed that serious fungal infections — particularly those that spread into the bloodstream — are associated with abnormal clotting.
According to a landmark study published in Blood, invasive aspergillosis is specifically “characterized by vascular invasion and thrombosis,” where the fungus physically invades blood vessel walls and sets off a clotting chain reaction.
A Japanese study published in FEMS Microbiology Letters found that proteinases secreted by Candida albicans directly activated clotting factors XII and X, as well as prothrombin — three critical proteins in the body’s coagulation cascade.
The researchers concluded that “peripheral and systemic blood circulation may be impaired by activation of the blood clotting cascade by microbial infections, especially in septic patients, which would enhance disseminated intravascular coagulation and multi-organ failure”.
Put simply: when fungi get into the bloodstream, they do not just cause infection — they can throw the body’s entire clotting system into chaos.
h2>
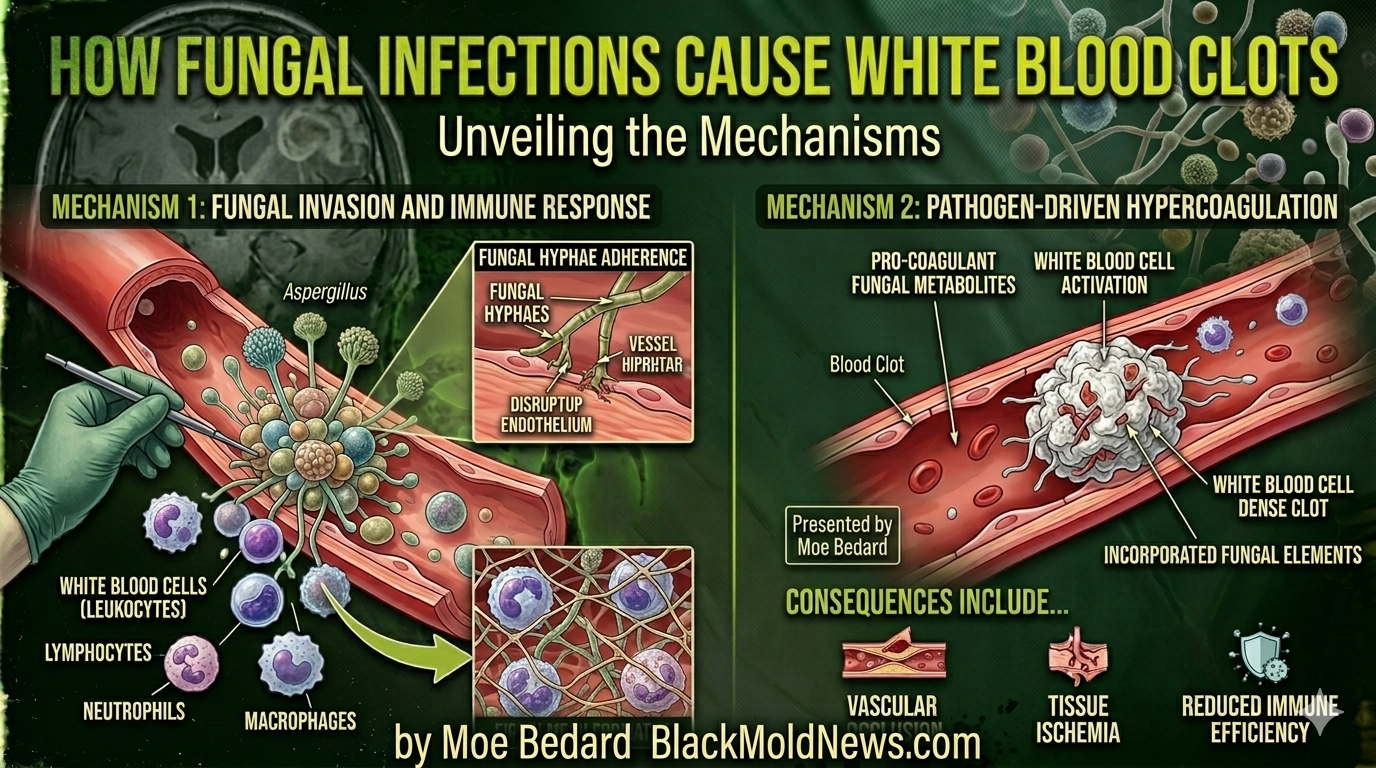
Fungal infections drive blood clots through three overlapping pathways. Understanding each one helps explain why these clots can be so severe and so hard to treat.
1. Direct Vascular Invasion
The most dramatic mechanism happens when fungal hyphae (the thread-like structures mold uses to grow) physically penetrate blood vessel walls. This is called angioinvasion, and it is a hallmark of Aspergillus fumigatus infections.
Research published in Blood showed that when A. fumigatus hyphae contact endothelial cells — the cells lining blood vessels — they trigger two devastating effects: direct cell injury and the surface expression of tissue factor, a protein that kicks off the blood clotting cascade.
Once tissue factor is expressed on the vessel wall, thrombin is generated, and fibrin clots form rapidly at the site of invasion.
A related study confirmed that vascular invasion by A. fumigatus also releases proinflammatory cytokines including IL-8 and TNF-α, further accelerating coagulation and causing ischemia — a shutdown of blood supply to nearby tissue. In invasive aspergillosis, this combination of thrombosis and tissue death can be fatal.
2. Enzyme-Driven Coagulation Activation
Many pathogenic fungi secrete powerful enzymes called proteinases. In Candida and related species, these enzymes can directly activate clotting factors in human blood.
Research into mucormycosis — a deadly infection caused by the Mucor family of molds — found an even more alarming mechanism.
The fungus secretes a subtilisin-like proteinase (called Arp) that not only activates fibrinogen (a clot-building protein) but also inactivates antithrombin III, the body’s primary anticoagulant “off switch”. With the brake system disabled, clotting runs unchecked.
This explains why mucormycosis regularly causes thrombotic occlusion of blood vessels, followed by tissue necrosis and gangrene in affected areas.
3. Mycotoxin-Induced Coagulation Disruption
You do not need a full-blown systemic fungal infection to affect the blood. Mycotoxins — the toxic chemical compounds produced by molds like Stachybotrys (black mold), Fusarium, and Aspergillus — can disrupt normal coagulation even without fungal cells in the bloodstream.
A study published in PubMed examined fusaric acid, a mycotoxin produced by Fusarium species commonly found in water-damaged buildings.
Researchers found that at low concentrations, fusaric acid shortened clotting time dramatically — dropping plasma recalcification time from 130 seconds to 32 seconds — suggesting a pro-clotting effect.
This kind of disruption to normal clotting balance could contribute to unexplained clotting events in people with significant mold exposure.
Research into aflatoxin — produced by Aspergillus flavus — showed that high doses disrupted the intrinsic coagulation pathway by suppressing factor VIII and factor IX activity.
This illustrates that different mycotoxins can push the clotting system in different directions: some toward dangerous clotting, others toward abnormal bleeding.
When fungal infections reach the bloodstream — a condition called fungemia or candidemia — the most feared clotting complication is disseminated intravascular coagulation (DIC).
DIC is a paradoxical condition where widespread, uncontrolled clotting throughout the body’s small blood vessels exhausts the supply of clotting factors, ultimately leading to simultaneous clotting and bleeding.
The Cleveland Clinic describes DIC as a rare but serious disorder triggered by conditions like sepsis and severe infections.
Research presented in the American Society of Hematology journal found that “candidemia can cause coagulation dysfunction and hyperfibrinolysis in hematologic malignancies and hematopoietic stem cell transplant patients”.
Candida sepsis-linked DIC has been documented in the medical literature since the early 1970s, with a case report identifying Candida albicans septicemia as a direct cause of DIC.
A 2021 NIH review further explained the molecular chain of events: fungal-triggered inflammation causes tissue factor release from endothelial cells, which overwhelms normal anticoagulant defenses, leading to what researchers describe as a “thrombin burst” — a flood of clot-generating activity across multiple organ systems
What Happens Inside Blood Vessels
To understand why this matters, picture the inner lining of a blood vessel — smooth, intact, and designed to keep blood flowing freely. When a Candida or Aspergillus infection reaches the bloodstream, what follows is a rapid series of damaging events:
-
Fungal adhesion — The organism attaches to the endothelial wall using surface proteins
-
Cell penetration — Hyphae or yeast forms are endocytosed (taken inside) by endothelial cells
-
Tissue factor expression — The injured endothelial cells signal the coagulation cascade to begin
-
Thrombin generation — Fibrin begins to form, trapping platelets and building a clot
-
Cytokine storm — Inflammation amplifies the coagulation signal, creating a vicious cycle
-
Vessel occlusion — Blood flow stops; downstream tissue dies from ischemia
This process can unfold in hours in immunocompromised patients and can lead to stroke, pulmonary embolism, organ failure, or death.
NETs: The Immune System’s Double-Edged Sword
There is another layer to this story that scientists are still uncovering. When the immune system detects fungal invaders, specialized white blood cells called neutrophils sometimes release web-like structures called neutrophil extracellular traps (NETs).
These structures are designed to catch and kill pathogens.
The problem is that NETs are also potent activators of the clotting cascade. Research published in PubMed found that NETs contribute to thrombosis, ischemia, and adverse cardiovascular events — and that circulating NET markers are associated with prothrombotic activity.
In severe fungal infections, the body’s own immune defenses can contribute to the blood clots that put patients at risk.
Conclusion
The science is clear: fungal infections are not just respiratory or skin conditions — they can reach into the blood itself, triggering dangerous clotting events through multiple biological mechanisms.
Whether through direct vascular invasion by Aspergillus, enzyme-driven coagulation activation by Candida, or mycotoxin-induced platelet disruption from environmental molds, the relationship between fungal biology and blood clotting is well-established in medical literature.
For people living or working in mold-contaminated buildings, this science underscores why prompt remediation and proper medical evaluation are not optional.
Mold is not just an aesthetic problem or a respiratory nuisance. In the right conditions, it can alter the fundamental chemistry of your blood.
Awareness is the first step. Clean air, dry buildings, and informed physicians are the solution.
References
-
Lopes-Bezerra, L.M. & Filler, S.G. (2004). Interactions of Aspergillus fumigatus with endothelial cells. Blood, 103(6), 2143–2149. https://pubmed.ncbi.nlm.nih.gov/14630829/
-
Kaminishi, H. et al. (1994). Activation of blood clotting factors by microbial proteinases. FEMS Microbiology Letters, 121(3), 327–332. https://pubmed.ncbi.nlm.nih.gov/7926688/
-
Müller, F.M. (2001). Blood coagulation in domestic deep-seated mycoses. PubMed. https://pubmed.ncbi.nlm.nih.gov/12073564/
-
Kannan, S. et al. (2013). Fusaric acid, a mycotoxin, and its influence on blood coagulation. PubMed. https://pubmed.ncbi.nlm.nih.gov/23343693/
-
Strickler, A. & Gingold, M. (1987). Hematologic manifestations of bacterial and fungal infections. PubMed. https://pubmed.ncbi.nlm.nih.gov/3308820/
-
Ben-Ami, R. et al. (2009). Aspergillus fumigatus inhibits angiogenesis through the production of gliotoxin. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC2925388/
-
Candida septic thrombosis of great central veins. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC1250982/
-
Cerebral Venous Thrombosis in Cryptococcal Meningitis. PubMed (2025). https://pubmed.ncbi.nlm.nih.gov/41443253/
-
Disseminated Intravascular Coagulation – Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/21836-disseminated-intravascular-coagulation-dic
-
Mold and Mycotoxin Exposure and Brain Disorders. IMR Press (2023). https://www.imrpress.com/journal/JIN/22/6/10.31083/j.jin2206137
-
Neutrophil Extracellular Traps in Cardiovascular Diseases. PubMed. https://pubmed.ncbi.nlm.nih.gov/38189504/
-
Disseminated Intravascular Coagulation – NIH/PMC (2025). https://pmc.ncbi.nlm.nih.gov/articles/PMC12143096/
-
Polarized Response of Endothelial Cells to Aspergillus fumigatus. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC3393649/
-
Pathological Blood Coagulation and the Mycotoxic Oxidative Stress Test. MedCrave. https://medcraveonline.com/IJVV/pathological-blood-coagulation-and-the-mycotoxic-oxidative-stress-testnbspmost.html


0 Comments